Heart failure most often goes undetected until a patient is acutely hospitalised, a costly and avoidable outcome. In primary care, even among high-risk individuals, the syndrome remains chronically missed. The PANACEA-HF study set out to change that by asking a deceptively simple question: can practice nurses be trained to bring AI-powered cardiac imaging directly into the primary care setting?
PANACEA-HF (Practice Nurses to Augment the Clinical Evaluation and cAre of people at high-risk of Heart Failure) is a prospective, pragmatic, multicentre surveillance study and nested RCT conducted across metropolitan and rural-remote primary care clinics in Australia. Practice nurses with no prior imaging experience were trained over six months to apply AI-mediated portable cardiac ultrasound (AI-PoCUS), acquiring detailed cardiac images across parasternal long-axis and apical chamber views, with colour Doppler and tissue Doppler velocities.
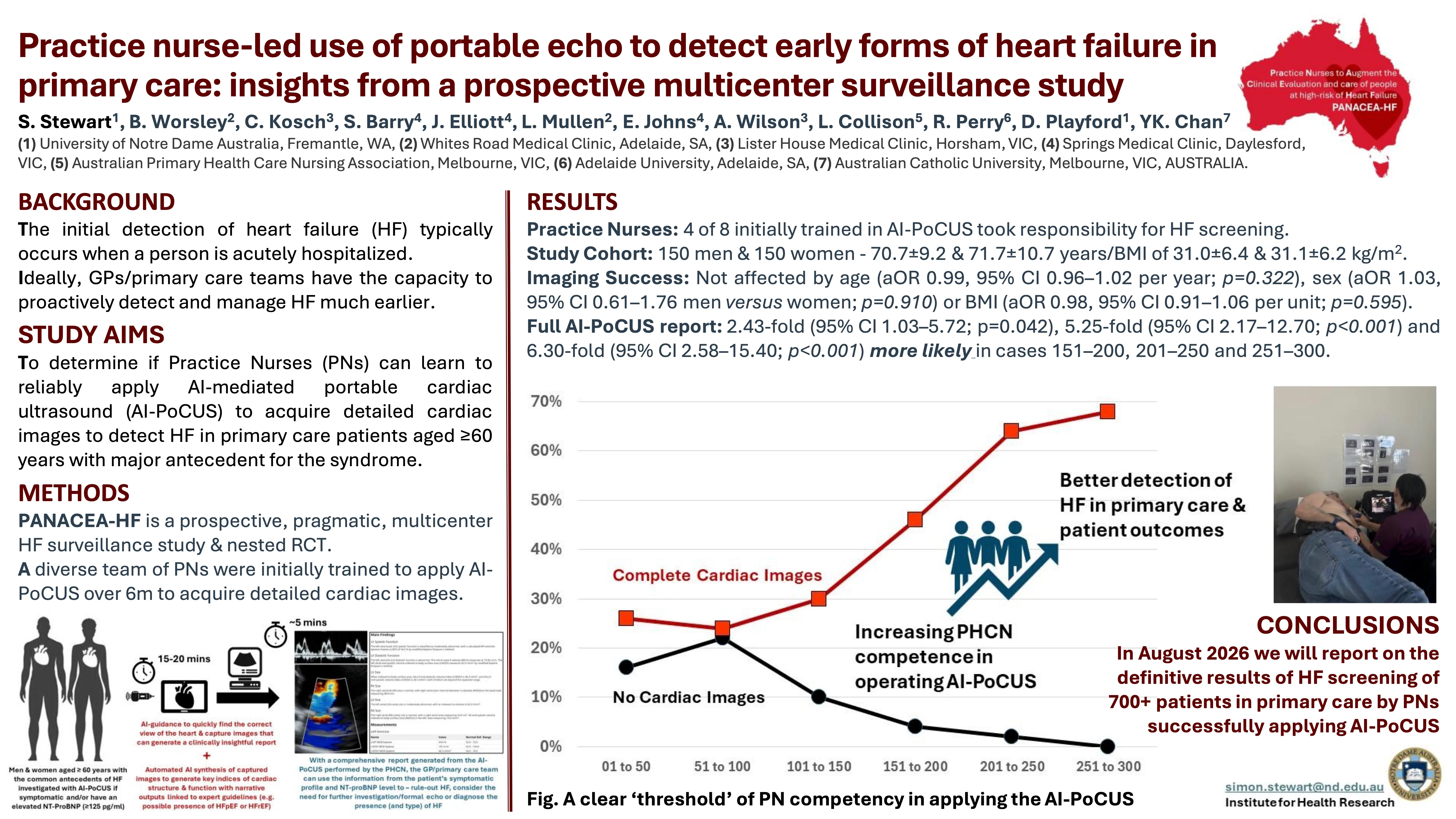
From the first 300 formally screened cases (150 men, 150 women; mean age ~71 years), a clear learning curve emerged and with it, a clear threshold of competence. Imaging failure rates dropped from 16% in the first 50 cases to zero in the final 50, while the rate of complete AI-PoCUS reports generating more than 30 cardiac indices rose from 26% to 68%. Imaging success was not influenced by patient age, sex, or BMI; the gains were driven entirely by nurse experience.
Key findings
- 4 of 8 trained practice nurses took on independent HF screening responsibility
- Imaging failure fell from 16% to 0% across the first 300 cases screened
- Complete AI-PoCUS reports (>30 cardiac indices) rose from 26% to 68%
- A clear competence threshold emerged after 30–40 screenings per nurse
- Full report generation was 6.30-fold more likely by cases 251–300 vs the first 50 (p<0.001)
- Imaging success was unaffected by patient age, sex, or BMI
Implications
These findings demonstrate that practice nurses, with structured training and ongoing support, can reliably generate clinically meaningful cardiac imaging as part of a proactive heart failure surveillance program. The PANACEA-HF model has direct implications for closing the gap in early HF detection at primary care level, particularly in rural and remote communities where specialist access is limited. Full results from screening of 700+ patients are expected in August 2026.