Overview
Breathlessness affects 10% of the adult population and over 25% of those aged above 70, yet diagnostic delays remain common, particularly in socioeconomically deprived communities where access to specialist services is limited. Heart failure and COPD together account for more than two thirds of breathlessness causes, and delays in diagnosis lead to worse outcomes, increased hospital admissions, and higher healthcare costs.
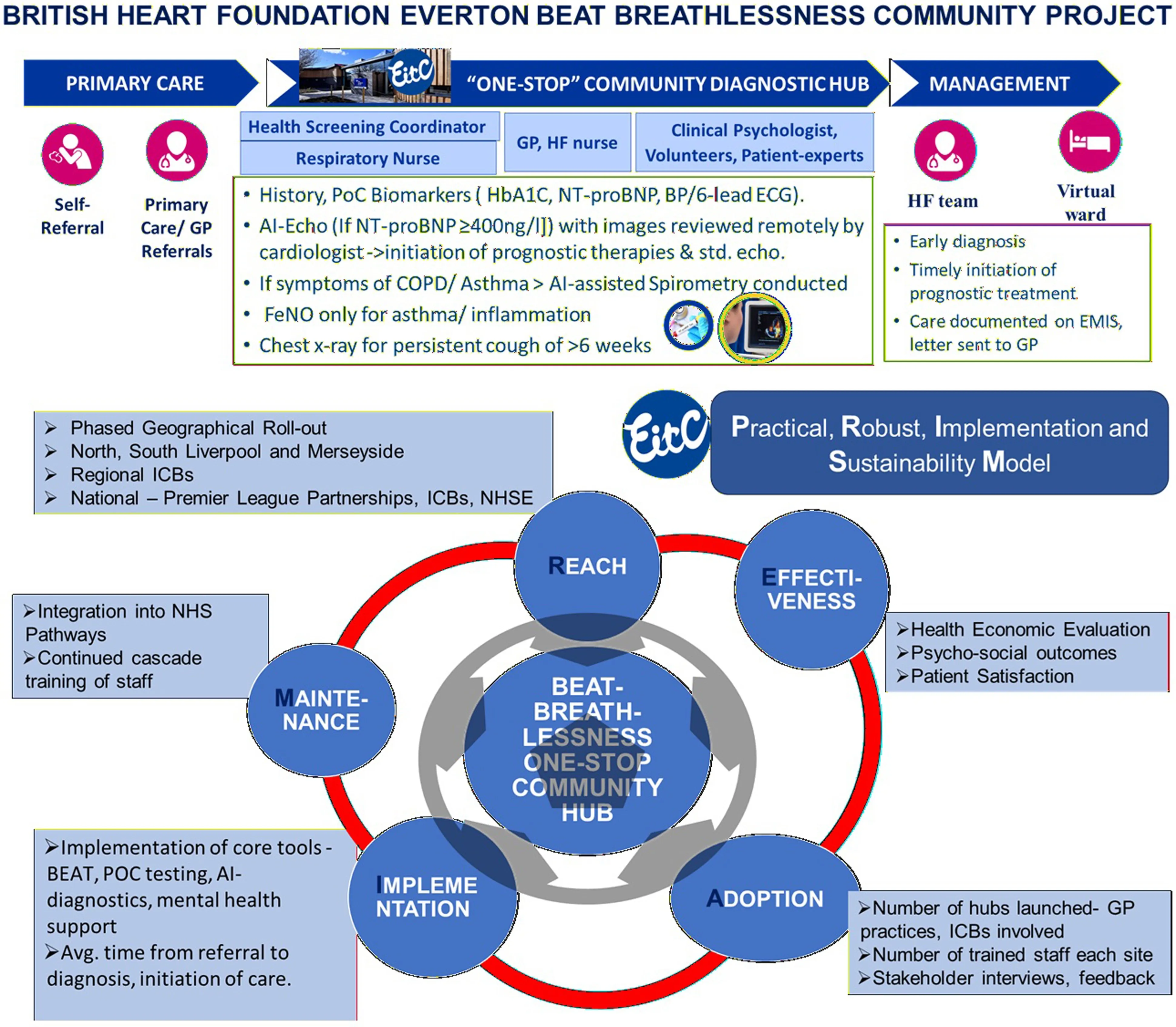
The Everton BEAT Breathlessness Project is a novel, community-based programme designed to close that gap. Funded by the British Heart Foundation Healthcare Implementation Fund, it brings together NHS providers, Everton in the Community (the charitable arm of Everton Football Club), the Pumping Marvellous Foundation, public health organisations, and Liverpool City Council to deliver accessible diagnostics in one of England's most deprived areas. This paper describes the programme's design, implementation methodology, and evaluation framework.
Project Design and Setting
The hub operates out of EitC's The People's Place, a mental health and wellbeing facility adjacent to Goodison Park in North Liverpool. The deliberate choice of a non-clinical, community-trusted venue reduces stigma and encourages engagement from individuals who may not present to traditional healthcare settings.
The programme targets adults aged over 40 experiencing breathlessness, exhaustion, or ankle swelling, recruited through self-referral, primary care referrals, and community outreach. Building on a successful 2024 pilot that identified new heart failure in 3% and new COPD in 12% of attendees, the expanded programme aims to screen 1,500 patients over 12 months across multiple sites in Liverpool and the wider Cheshire and Merseyside region.
The Role of US2.ai
US2.ai sits at the centre of the clinical pathway as the AI-assisted echocardiography platform. Patients who present with relevant symptoms and an elevated point-of-care NT-proBNP (400 pg/mL or above) proceed to an AI-assisted echo, with images acquired by trained heart failure specialist nurses or general practitioners under cardiologist oversight.
The platform enables comprehensive cardiac assessment without requiring an on-site echocardiographer, making guideline-directed diagnostic quality achievable in a community setting. Once heart failure is confirmed, prognostic guideline-directed medical therapy is initiated with a target of assessment and treatment within 60 minutes of arrival, a model the programme calls BEAT to Treat in 60 Minutes.
Integrated Diagnostic Pathway
Alongside AI-assisted echocardiography, the one-stop hub offers a concurrent suite of assessments including AI-spirometry for COPD, FeNO testing for asthma, KardiaMobile 6-lead ECG for atrial fibrillation, blood pressure checks, smoking cessation support, and anxiety screening. A clinical psychologist advises on breathlessness and anxiety interactions, reflecting the programme's whole-person approach.
Confirmed diagnoses feed directly into specialist clinical pathways including heart failure clinics, virtual wards, and pulmonary rehabilitation, with care documented and communicated back to primary care.
Evaluation and Scale
The programme is assessed using a mixed-methods framework measuring diagnostic yield, time from symptom onset to diagnosis, quality of life, hospital admissions, and cost savings. Health equity is tracked through deprivation index analysis. The target is 125 screening sessions per month across multiple sites.
Results will be disseminated through peer-reviewed publications and a replication toolkit designed to support rollout to other NHS sites and Premier League club partnerships nationally.
Why This Matters
This programme demonstrates that US2.ai can be deployed effectively beyond the hospital, enabling high-quality cardiac diagnostics in community environments by non-specialist operators. It represents a real-world implementation model for reducing health inequalities through AI-assisted technology, reaching populations who would otherwise face delayed or missed diagnoses.
Related Publication
For the initial results from the programme, see the pilot study published in JACC Heart Failure (2025).
Sankaranarayanan, R., Hartshorne-Evans, N., Lip, G. Y. H., & the Everton BEAT Breathlessness Team. (2026). British Heart Foundation-funded programme: breathlessness hub in Liverpool. European Heat Journal, ehag279. https://doi.org/10.1093/eurheartj/ehag279